Our research projects
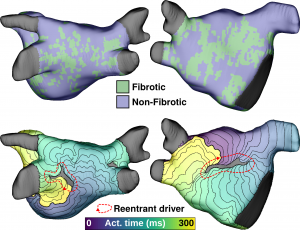 Simulations conducted in computational models reconstructed from MRI scans at clinical resolution have emerged as a powerful new tool in the clinical arsenal for treating cardiovascular disease and stratifying risk of future incidents (e.g., sudden cardiac arrest, stroke). Projects include:
Simulations conducted in computational models reconstructed from MRI scans at clinical resolution have emerged as a powerful new tool in the clinical arsenal for treating cardiovascular disease and stratifying risk of future incidents (e.g., sudden cardiac arrest, stroke). Projects include:
- Better understand mechanisms interconnecting fibrosis, fibrillation, and stroke in patients with atrial cardiomyopathy
- Quantifying sources of uncertainty in computational simulations of the heart to enable more effective model validation and verification
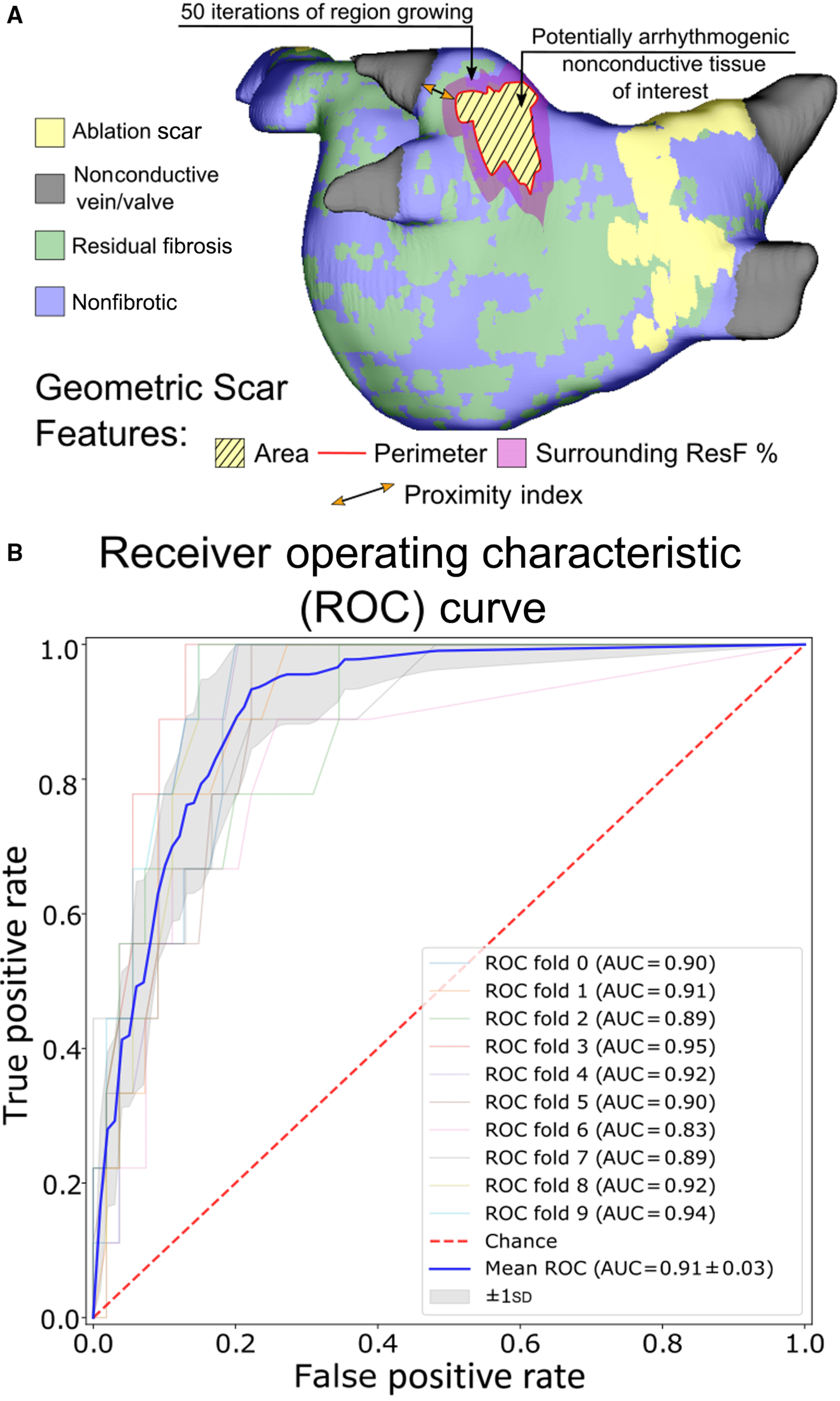
- Predicting optimal ablation targets in patients with complex arrhythmias
- Developing new frameworks for efficient and clinically useful assessment of arrhythmia susceptibility in patient-specific cardiac models
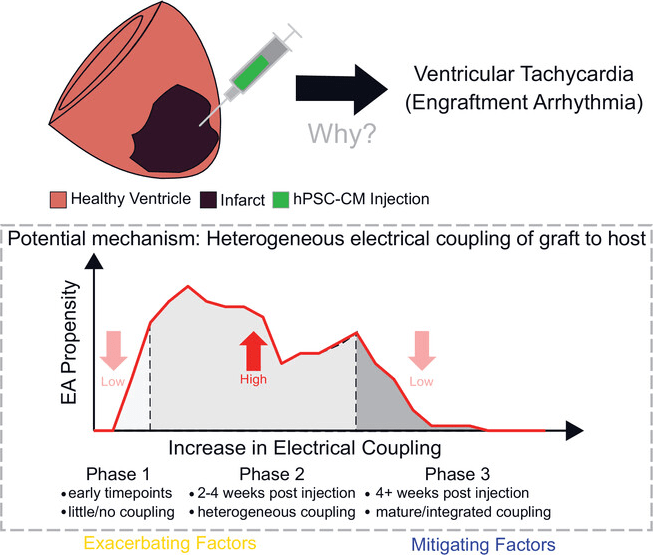
Tachyarrhythmias that occur following injection of heart-like cells derived from stem cells (hPSC-CM) are a huge hindrance to the feasibility of translating this exciting technology to clinical applications. Computational heart models have emerged as a powerful tool for deciphering this type of relationship.
Projects include:
- Understanding sources of triggered arrhythmia following hiPSC-CM implantation in vivo
- Characterizing the efficacy and safety of specific cell injection patterns
hiPSC-CM can also be used as a means of modeling genetically inherited conditions that cause rhythm disorders. The lab is currently embarking on a new research trajectories that will involve using measurements from individual patients’ hiPSC-CM as a means of personalizing cell- and tissue-scale electrophysiological parameters in organ-scale models.
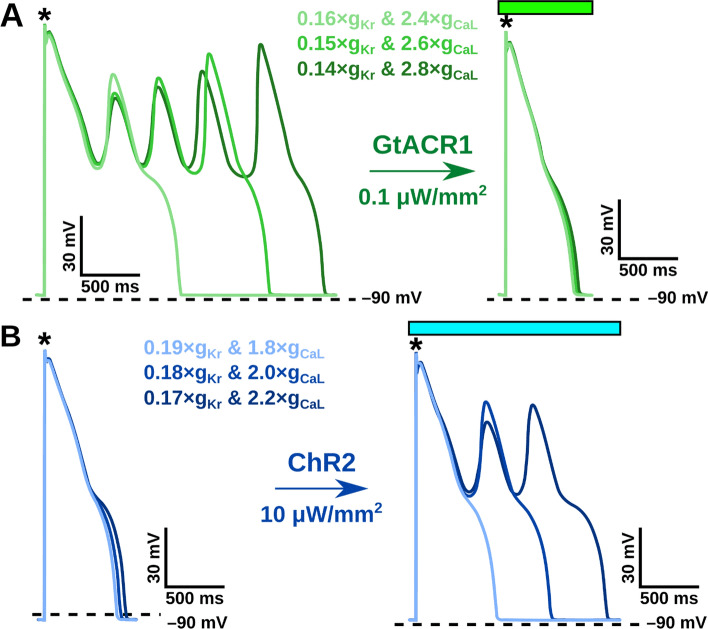 Work in this area has led to the development of a robust computational framework for modeling optogenetics in the heart. This methodology enables simulations that can help understand how light could be used to treat arrhythmia. There is a high level of public excitement about cardiac optogenetics and great enthusiasm for further research along this trajectory.
Work in this area has led to the development of a robust computational framework for modeling optogenetics in the heart. This methodology enables simulations that can help understand how light could be used to treat arrhythmia. There is a high level of public excitement about cardiac optogenetics and great enthusiasm for further research along this trajectory.
Projects include:
- Using optogenetic tools to scale mechanistic insights from mouse experimental models of arrhythmia to better understand human cardiac physiology
- Developing simulations to help forecast and shape the future development of devices that might change the way arrhythmia is treated (e.g., via incorporation of new opsin variants like anion channelrhodopsins and other emerging novel constructs)
- Using optogenetics to modulate propensity for afterdepolarization-mediated ectopic beats
 The lab’s most recent endeavor is to use artificial intelligence and machine learning (AI/ML) to pinpoint patients at risk for specific adverse cardiac outcomes using single ECG recordings, echocardiograms, MRI scans, or multi-variable, multi-modal clinical data. Identifying patients most in need of care allows clinicians to monitor and provide treatment, potentially reducing unnecessary testing. AI/ML has been used successfully in similar areas, such as identifying patients with atrial fibrillation using ECGs acquired in the absence of arrhythmia. We are particularly interested in the development and application of tools to facilitate better explainability and interpretability of AI/ML methods, which we expect to hasten the process of clinical translation.
The lab’s most recent endeavor is to use artificial intelligence and machine learning (AI/ML) to pinpoint patients at risk for specific adverse cardiac outcomes using single ECG recordings, echocardiograms, MRI scans, or multi-variable, multi-modal clinical data. Identifying patients most in need of care allows clinicians to monitor and provide treatment, potentially reducing unnecessary testing. AI/ML has been used successfully in similar areas, such as identifying patients with atrial fibrillation using ECGs acquired in the absence of arrhythmia. We are particularly interested in the development and application of tools to facilitate better explainability and interpretability of AI/ML methods, which we expect to hasten the process of clinical translation.
Our most exciting funded project in the AI/ML space relates to the use of echocardiography data from childhood cancer survivors to predict the onset of cardiovascular disease. Kids who endure cancer treatment have lifetime risk of cardiomyopathy and heart failure, but it can be hard to know when these events will take root. Better early warning systems enabled by AI/ML will pave the way towards better and more equitable treatment regimes.
